In 1998 there were:
By contrast,
Routine chest x-ray screening often are unable to detect lung cancers until they are of advanced stage.
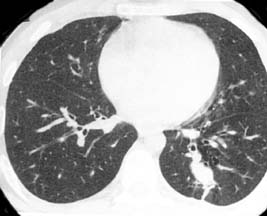
A study by Henschke, et al.found that non-calcified pulmonary nodules were detected in 23% participants by low dose CT at baseline, compared with 7% by chest radiography. Malignant disease was detected in 2-7% by CT and of the 27 CT-detected cancers, 26 were resectable. It was concluded that low-dose CT can greatly improve the likelihood of detection of small (early) lung cancers, and thus potentially more curable stage.
Effective in 2015, Medicare guidelines will now cover annual low dose CT lung cancer screening for enrollees who meet all of the following criteria: they are age 55 to 74 years old; and are either current smokers or have quit smoking within the last 15 years; have a tobacco smoking history of at least 30 “pack years” (an average of one pack a day for 30 years); and they receive a written order from a physician or qualified non-physician practitioner that meets certain requirements.
Diagnostic Chest CT scans require a prescription by a physician and will only be reimbursed by insurance companies if strict criteria are met. Usually this test is performed if there is an abnormal chest x-ray or history of cancer. Diagnostic CT Scans of the Chest are ordered as a problem solving modality, and usually necessitate intravenous administration of iodinated contrast.
Low-Dose Screening CT is intended to supplement or replace routine CXRs which are performed in patients without symptoms or known disease. Like screening mammography, it is essential to minimize the amount of radiation exposure in asymptomatic patients. The test is specifically designed to rapidly screen the lungs with minimal radiation exposure, to allow detection of pulmonary nodules. No intravenous contrast is used.
Low-Dose Screening CT is specifically designed to screen for pulmonary nodules, and is neither designed nor intended to screen for abnormalities elsewhere in the thorax (ie- heart, aorta, lymph nodes, bones).
Since this is a screening test, some insurance companies may not reimburse for its cost.
Since it is critical to minimize radiation and to provide complete lung coverage in a breathhold, this test should only be performed on a helical (spiral) CT scanner with current software and hardware upgrades.
First, you complete a brief risk factor questionnaire. Next, you lie down on the imaging table and a CT technologist will ask you to hold your breath while the images are taken. That's it. In twenty seconds, your exam is complete, and you may return to your regular routine. The procedure is pain free, non-invasive, and inexpensive.
Your examination will be overread by two board certified radiologists, and results will be sent to you and your doctor within 48 hours.
If your test was read as negative, then no pulmonary nodules were detected. If you are at high risk for lung cancer, then you should consider repeating the exam yearly.
If the radiologists detected a pulmonary nodule that raises concern, then you will be urged to make an appointment with a lung specialist. You may be asked to return for a diagnostic CT Chest, which is performed with higher spatial resolution and thin cuts through areas of concern, allowing characterization of nodules detected by the screening exam. Frequently, nodules detected on the screening exam are subsequently revealed to be benign granulomas or scars on the diagnostic study. Therefore, an initially positive screening test does not necessarily mean that you have lung cancer.
Henschke CI, et al. Early Lung Cancer Action Project: overall design and findings from baseline screening. The Lancet 1999:354:99-105.