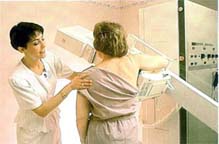
Digital Mammography.This safe, low-dose x- ray of the breast is a crucial tool in helping to discover small cancers. Digital mammography improves the radiologist's ability to read mammograms, as there is improved contrast between normal and abnormal tissues making diagnosis easier.
Digital Tomosynthesis, aka "3D" mammography, is an exciting new technology for the diagnosis of breast cancer. The mammographic detectors 'sweep' along the breast as the images are acquired, creating a set of images that allow a radiologist to 'see through' overlapping tissue, which is a limitation in conventional mammography. This allows for better visualization of underlying lesions, and a decrease in 'false positive' mammograms which lead to unnecessary additional imaging. The women's imaging experts at Boca Radiology have extensive experience with tomosynthesis, and have utilized it in both screening and diagnostic arenas.
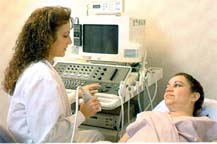
This procedure uses sound waves to provide pictures of suspicious areas in the breast. Ultrasound is a powerful technique and has been demonstrated to identify lesions which can be 'hidden' on mammography. However, it is best used in conjunction with conventional mammography, and not a replacement, as mammography can still find lesions that are not easily seen on ultrasound.
Magnetic Resonance Imaging is a radiation-free procedure that provides detailed functional breast imaging, further defining lumps an pinpointing size and location. It works on the principle of cancers have abnormal increased blood flow. Patients are injected with gadolinium agent, a type of IV contrast, and multiple images are taken. MRI is a very powerful tool and has a very high sensitivity. Its best used as a screening tool in patients with high-risk (patients with genetic mutations or strong family history) or as staging exam for patients with newly diagnosed breast cancer. MR can also help physicians evaluate breast implants.
Positron Emission Mammography is another 'functional imaging' modality, that uses F18 labeled glucose to map metabolically active tumors. Essentially its a PET scan for the breast. We have extensive experience with PEM and have had our PEM research published in major peerreviewed journals, such as Radiology. Our experience and volume allows us to be involved in education, hosting visiting radiologists who enroll in our PEM fellowship.
Molecular breast imaging is the newest technology we offer in the diagnosis and imaging of breast cancer. This test involved the intravenous injection of Technetium 99, a nuclear medicine imaging agent, which then localized to metabolically active tissues and tumors. The modality is best used as an adjuvant to mammography in intermediate risk patients or as an alternative to MRI in patients who have contraindications to MRI.
Imaging Guided Procedures
Once an abnormality is found on imaging, it may be necessary to perform an imageguided biopsy. As fellowship trained subspecialists, we perform many of these biopsies and procedures every day and have been involved with educating visiting physicians on these procedures.
Ultrasound Guided Needle Biopsys
If an abnormality that needs biopsy is seen on ultrasound, this is the prefered method of biopsy. With a very thin needle, physicians can remove enough cells and/or fluid from palpable or non-palpable masses to help determine if they are cancerous. We utilize a variety of vacuum-assisted core needle biopsies, such as the Mammotome, Atec, and Precise biopsy needles.
Non-surgical, Digital Stereotactic Breast Biopsy.
Occasionally a finding which needs to be biopsied is only visible on mammography, such as in the case for microcalcifications. In those instances, a stereotactic biopsy would be needed. This type of biopsy uses a computer to help target a finding for biopsy under mammographic guidance. In presence of a Faxitron in the room allows us to determine if an adequate sample was taken.
If a finding is only visible on MRI, then an MRI guided biopsy would be needed. We are one of the first centers in South Florida to have started an MRI biopsy program, and have trained visiting radiologists in this procedure from all over the world.
There are very few centers and physicians in the country that have as much experience with PEM as we have. Even fewer have the ability and experience of the many PEM-guided biopsy that we have. In certain cases, we can even perform the biopsy at the time of imaging, which can alleviate the need to have to be imaged twice.
This is an exciting new procedure we are pleased to introduce to the community. In the past, when a patient was to undergo surgical excision or excisional biopsy, the area in question needed to be 'localized' with a wire for the surgeon. Wire localizations needed to be performed the day of surgery and can be inconvenient for the patient. Additionally, the surgeon is confined to the wire track for excision. With radioactive seed localization (RSL), a small radiation seed is implanted in the breast the day before the surgery. No wires are left protruding from the breast. Patients can show up to their surgery at a more convenient time. Surgeons are no longer 'hand-cuffed' to the track of the wire and can take any approach for excision they deem appropriate.
Occasionally a patient will need an excisional biopsy of a finding only seen on MRI instead of a needle biopsy. In those instances, we can localize the MRI finding and place a wire through the finding, which helps map the finding so the surgeon can localize the lesion for surgery.
As part of surgical treatment for breast cancer, patients undergo sentinel lymph node biopsy for staging. While the patient is on the operating table for their lumpectomy or mastectomy, a sample of the 1st draining lymph nodes in the axilla ("armpit") are removed and assessed for any spread of cancer. If negative, no further lymph nodes need to be removed, sparing the patient the potential complications that can occur with a full axillary dissection. To help identify those 1st draining nodes, the radiologist injects radioactive tracer intradermally around the nipple the day of surgery, which then localizes to the initial 'sentinel nodes', allowing them to be identified. By changing the type of radiotracer we use, we have found that patients have tolerated the procedure much better than in the past.
Combining a highly trained staff with the most advanced technology,
the Center for Breast Care of Boca Raton Regional Hospital provides several options for diagnosis.
Our revolutionary team approach ensures quality,focused attention to each patient's individual needs. It's part of our commitment to putting patients first.

the Center for Breast Care
at The Women's Center
of Boca Raton Regional Hospital,